  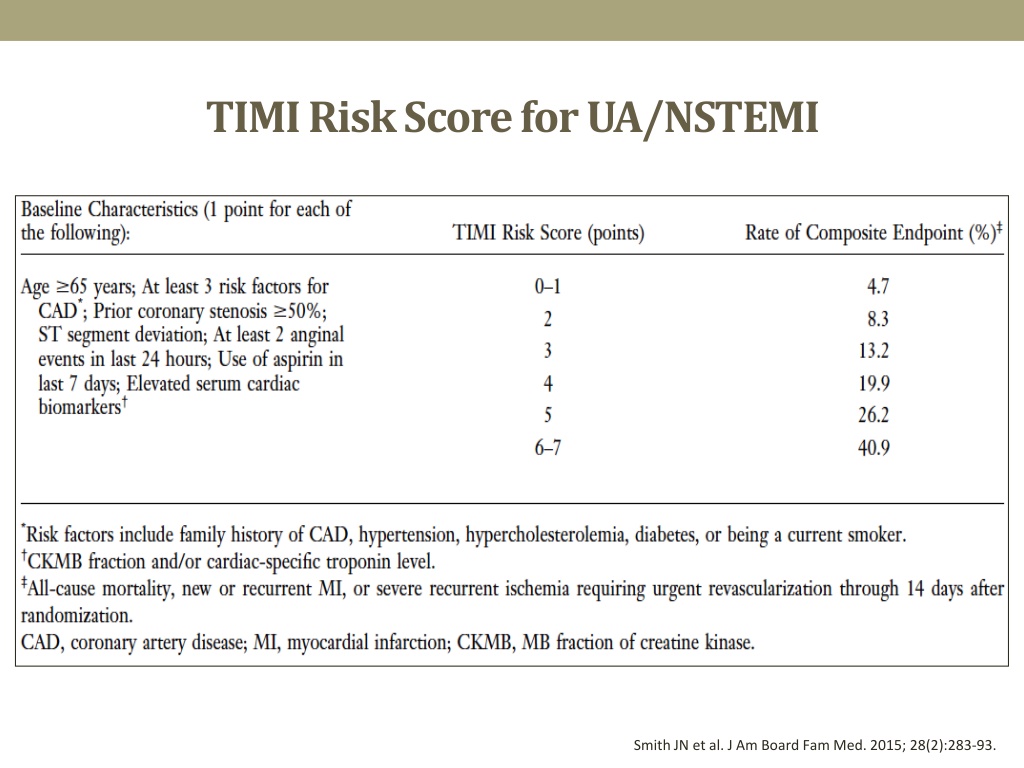
Across both trials, the benefit of an early invasive strategy was significantly greater with increasing baseline risk: OR, 1.39 in low-risk, 0.80 in intermediate-risk, and 0.57 in high-risk patients (P< or =0.004 for interactions). Compared with patients in TIMI IIIB and adjusting for baseline risk, patients in TACTICS-TIMI 18 had lower rates of death, MI, or rehospitalization for acute coronary syndromes (OR, 0.62 P<0.0001). Within each risk category, the rates of clinical outcomes and the benefit of an early invasive strategy were compared. Patients were stratified on the basis of their TIMI risk score into low-, intermediate-, and high-risk categories. We sought to examine the effect of these advances on clinical outcomes and the benefits of an early invasive strategy in UA/NSTEMI. TIMI risk can be calculated on the TIMI website under "Clinical Calculators.TIMI IIIB and TACTICS-TIMI 18 were 2 trials of an early invasive strategy in unstable angina (UA)/non-ST-elevation myocardial infarction (NSTEMI) that were conducted nearly a decade apart but with virtually identical enrollment criteria and designs, except that upstream glycoprotein IIb/IIIa inhibition was mandated and coronary artery stenting was routinely used in TACTICS-TIMI 18. 'TIMI risk' estimates mortality following acute coronary syndromes. 1 Pointĥ% risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization.Ĩ% risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization.ġ3% risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization.Ģ0% risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization.Ģ6% risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization.Ĥ1% risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization. % risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization. *Risk factors include: family history of CAD, hypertension, hypercholesterolemia, diabetes, or being a current smoker. Severe angina (≥ 2 episodes w/in 24 hrs).Known coronary artery disease (CAD) (stenosis ≥ 50%).TIMI Score Calculation (1 point for each): In patients with UA/NSTEMI, the TIMI risk score is a prognostication scheme that categorizes a patient's risk of death and ischemic events and provides a basis for therapeutic decision making. Among the group's most important works is the TIMI Risk Score, which assesses the risk of death and ischemic events in patients with unstable angina (UA) or non-ST elevation myocardial infarction (NSTEMI). Braunwald held the chairmanship until 2010, when he appointed Marc Sabatine to the position. The TIMI Study Group was founded by physician Eugene Braunwald in 1984. The group has its headquarters in Boston, Massachusetts. The Thrombolysis In Myocardial Infarction ( TIMI) Study Group, is an academic research organization (ARO) affiliated with Brigham and Women's Hospital and Harvard Medical School with a focus in the field of cardiovascular disease. For other uses, see Timi (disambiguation). For the IBM technology, see IBM i § TIMI. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
